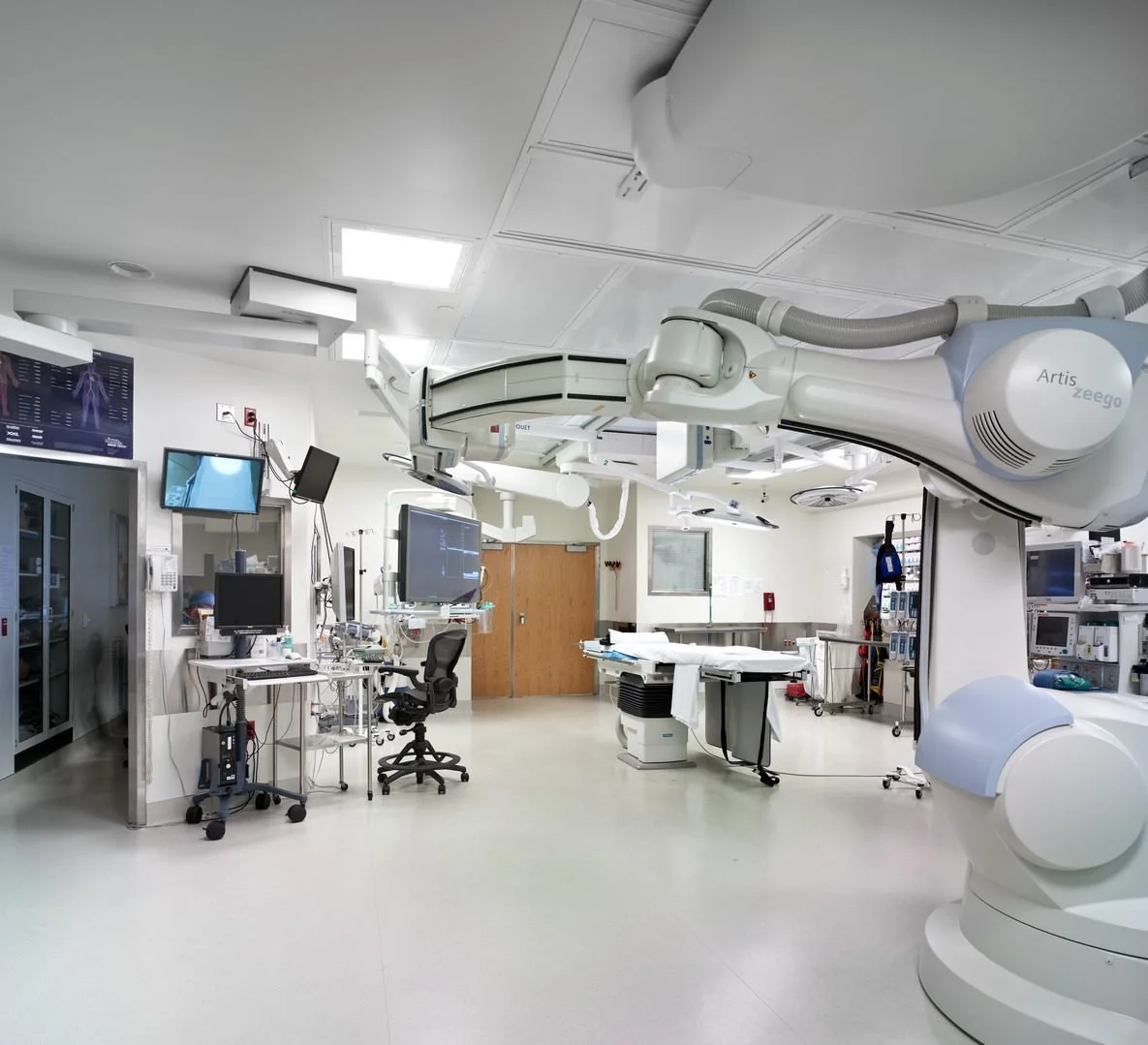
What Patients Don’t See Behind the Operating Room Doors
I myself had surgery recently that required general anesthesia. It was at the hospital I worked at and with people who were my friends and colleagues, yet it was still an intimidating experience. It got me thinking about all the things that go on for one operation to happen safely.
When most people think about surgery, they imagine a single moment: the surgeon standing over an operating table, making an incision, fixing a problem, and stitching things closed.
In reality, that moment is only a small part of a carefully choreographed process involving planning, preparation, technology, teamwork, and vigilance. Long before the first incision — and long after the last suture — dozens of steps take place to ensure safety, precision, and the best possible outcome.
As a general surgeon, I’ve always believed that patients feel more at ease when they understand what happens beyond the operating room doors. This article pulls back the curtain on the entire surgical journey: from preparing the room, to anesthesia, to equipment selection, to the operation itself, and finally to waking up safely in recovery.
Preparing the Operating Room: Setting the Stage
An operating room (OR) is not simply a sterile room with bright lights. It is a highly controlled environment designed to minimize infection, maximize efficiency, and ensure every team member has exactly what they need.
Preparation begins well before the patient arrives.
The Case Card: The Surgical Blueprint
Every surgery starts with a case card — essentially the surgical game plan. This document specifies:
The procedure being performed
The surgeon’s preferred instruments
Required implants or prosthetics
Special equipment
Suture types
Medications
Patient positioning needs
For example, if I’m performing a complex hernia repair using mesh, the case card will specify:
Type and size of mesh
Fixation devices or sutures
Specialized retractors
Energy devices for tissue dissection
Laparoscopic or robotic instruments if applicable
This ensures nothing is left to chance. When the patient enters the room, every necessary tool is already present, checked, and sterile.
Sterile Setup
Surgical technologists and nurses open instrument trays, sterile drapes, sutures, and implants. Every item is verified for:
Sterility indicators
Expiration dates
Integrity of packaging
Once opened, instruments are arranged in precise order so the surgical team can work efficiently without searching for tools mid-operation.
Equipment Checks
Modern surgery relies heavily on technology. Before each case, staff confirm proper functioning of:
Operating lights
Suction devices
Electrocautery units
Anesthesia machines
Monitors
Laparoscopic towers or robotic systems
Backup equipment is available in case of unexpected failure. Redundancy is part of safety.
Environmental Controls
Air filtration systems maintain positive pressure airflow to reduce infection risk. Temperature and humidity are regulated. Floors and surfaces are disinfected. Every detail matters.
By the time the patient enters the OR, the room is not merely “ready” — it has been meticulously engineered for safety.
The Anesthesia Setup: The Guardian of Comfort and Stability
While surgeons focus on the procedure, anesthesiologists focus on something equally critical: keeping the patient safe, comfortable, and physiologically stable.
Preparing the Anesthesia Station
Before the patient arrives, the anesthesia team:
Checks ventilators
Tests oxygen delivery systems
Prepares airway equipment
Draws up medications
Verifies emergency drugs
Ensures monitoring equipment is functioning
Every anesthesia machine undergoes a pre-use safety checklist. These checks are standardized and mandatory, not optional.
Monitoring Equipment
Once connected, patients are continuously monitored for:
Heart rhythm
Blood pressure
Oxygen levels
Carbon dioxide levels
Temperature
These metrics provide real-time insight into how the body responds to anesthesia and surgery.
Anesthesia is not simply “going to sleep.” It is a carefully controlled medical state, constantly adjusted moment by moment.
Bringing the Patient Into the OR
For patients, me included the trip into the operating room can be one of the most anxiety-provoking moments. For the surgical team, it is a carefully structured transition.
Identity and Procedure Verification
Before entering the OR, the team confirms:
Patient identity
Procedure to be performed
Surgical site and side
Allergies
Consent
This is repeated again once inside the OR — a process called the “time-out.” It ensures every person in the room agrees on exactly what will happen before any incision is made.
Positioning on the Operating Table
Once inside, the patient is moved onto the operating table. Positioning is not casual — it is a safety-critical step.
The team ensures:
Proper body alignment
Padding of pressure points
Protection of nerves
Secure straps to prevent falls
Appropriate positioning for surgical access
For example, abdominal surgery may require slight head-up positioning. Hernia repairs may require specific leg placement. Robotic surgery may involve steep positioning. Every posture is chosen to balance surgical access with patient safety.
Even small positioning errors can cause nerve injuries or pressure sores — which is why this step is taken so seriously.
Induction of Anesthesia: The Transition to Sleep
Once positioned and connected to monitors, anesthesia begins.
Induction
Medication is administered through an IV. Within seconds, the patient gently drifts off to sleep. Breathing is then supported through a breathing tube or airway device. Throughout the case, anesthesia continuously monitors and adjusts medications to maintain stable vital signs.
From the patient’s perspective, this moment feels like falling asleep. From the team’s perspective, it is a critical transition where physiology must be precisely controlled.
Once anesthesia confirms stability, surgery begins.
The Final Pre-Incision Safety Check: The Surgical Time-Out
Before any incision, the entire team pauses.
Out loud, they confirm:
Patient name
Procedure
Surgical site
Imaging availability
Antibiotic administration
Special equipment needs
This is a universal safety protocol designed to prevent wrong-site or wrong-procedure surgery. It may seem repetitive — but repetition saves lives.
Only after the time-out is complete does the surgeon begin.
Starting the Case: Controlled Precision
With the first incision, the visible part of surgery begins — but behind the scenes, constant coordination continues.
The surgical team includes:
Surgeon
Assistant or resident
Scrub technician
Circulating nurse
Anesthesia team
Each person has defined responsibilities. Instruments are passed seamlessly. Suction and cautery are adjusted. Fluids are administered. Vital signs are monitored continuously.
Equipment in Action
Depending on the procedure, equipment may include:
Energy devices to control bleeding
Laparoscopic cameras
Robotic arms
Specialized retractors
Surgical staplers
Mesh implants
Sutures of various materials and sizes
For example, in hernia repair, mesh selection is critical. The correct size and type must be chosen to reinforce the abdominal wall appropriately. Fixation may involve sutures, tacks, or glue depending on anatomy and technique.
These decisions are guided by experience, anatomy, and surgical judgment — often in real time.
Counts: Preventing Retained Objects
Throughout surgery, nurses perform instrument, needle, and sponge counts.
Counts occur:
Before incision
Before closing deep layers
Before final skin closure
If anything is missing, the team stops until it is found. X-rays are used if necessary. This process prevents retained surgical items — a rare but serious complication.
Counting is methodical, repetitive, and essential. It reflects the culture of shared responsibility in the OR.
Completing the Case: Closing with Intention
As the procedure concludes, attention shifts to reconstruction and closure.
Final Inspection
Before closing, the surgeon:
Checks for bleeding
Verifies repair integrity
Confirms correct placement of implants or mesh
Ensures no unintended injuries occurred
Only once satisfied does closure begin.
Layered Closure
Incisions are closed in layers to restore anatomy and minimize complications:
Deep fascial layers
Subcutaneous tissue
Skin
Suture choice depends on tissue type, tension, and healing properties. Sometimes staples or skin adhesives are used.
Dressings are applied. Drains may be placed if needed. Everything is documented.
The procedure itself may last minutes or hours — but precision remains constant.
Waking Up: Emergence from Anesthesia
As surgery ends, anesthesia gradually lightens sedation. The breathing tube is removed once the patient can breathe independently and safely.
This phase is delicate. The team monitors:
Breathing pattern
Oxygen levels
Blood pressure
Consciousness level
Once stable, the patient is transferred to a recovery bed.
Transport to the Recovery Room
The patient is moved to the post-anesthesia care unit (PACU), accompanied by anesthesia and nursing staff.
In recovery:
Vital signs continue to be monitored
Pain control is adjusted
Nausea is treated
Surgical sites are checked
Only once stable are patients discharged home or admitted to a hospital room.
After the Doors Close Again
Once the patient leaves the OR, work continues:
Instruments are reprocessed
The room is cleaned
Documentation is completed
Pathology specimens are sent
Surgeons speak with family members
Then the cycle begins again for the next patient.
Why This All Matters
For patients, surgery can feel like a leap of faith. You fall asleep, and when you wake up, something inside you has changed. What you don’t see is the immense preparation, redundancy, teamwork, and vigilance dedicated to your safety.
Every checklist.
Every piece of equipment.
Every count.
Every pause.
They exist for one purpose: to protect you.
Modern surgery is not just skill with a scalpel. It is system-based safety, communication, technology, and experience working together.
A Final Thought
As surgeons, we never forget that every patient on the operating table is someone’s parent, child, partner, or friend. Behind the sterile drapes and bright lights is a person placing enormous trust in the team.
That trust is earned through preparation, discipline, and constant attention to detail — long before the first incision and long after the final stitch.
So the next time you think about surgery, remember: what happens behind the operating room doors is far more than an operation. It is a carefully orchestrated commitment to your safety.